Acne Keloidalis Nuchae also called AKN
Acne Keloidalis Nuchae also called AKN : If You are interested in consulting Dr U for your Acne Keloidalis Nuchae (AKN), please fill out this form wit as much detail as possible: Free Online consultation form for Acne Keloidalis with Dr U
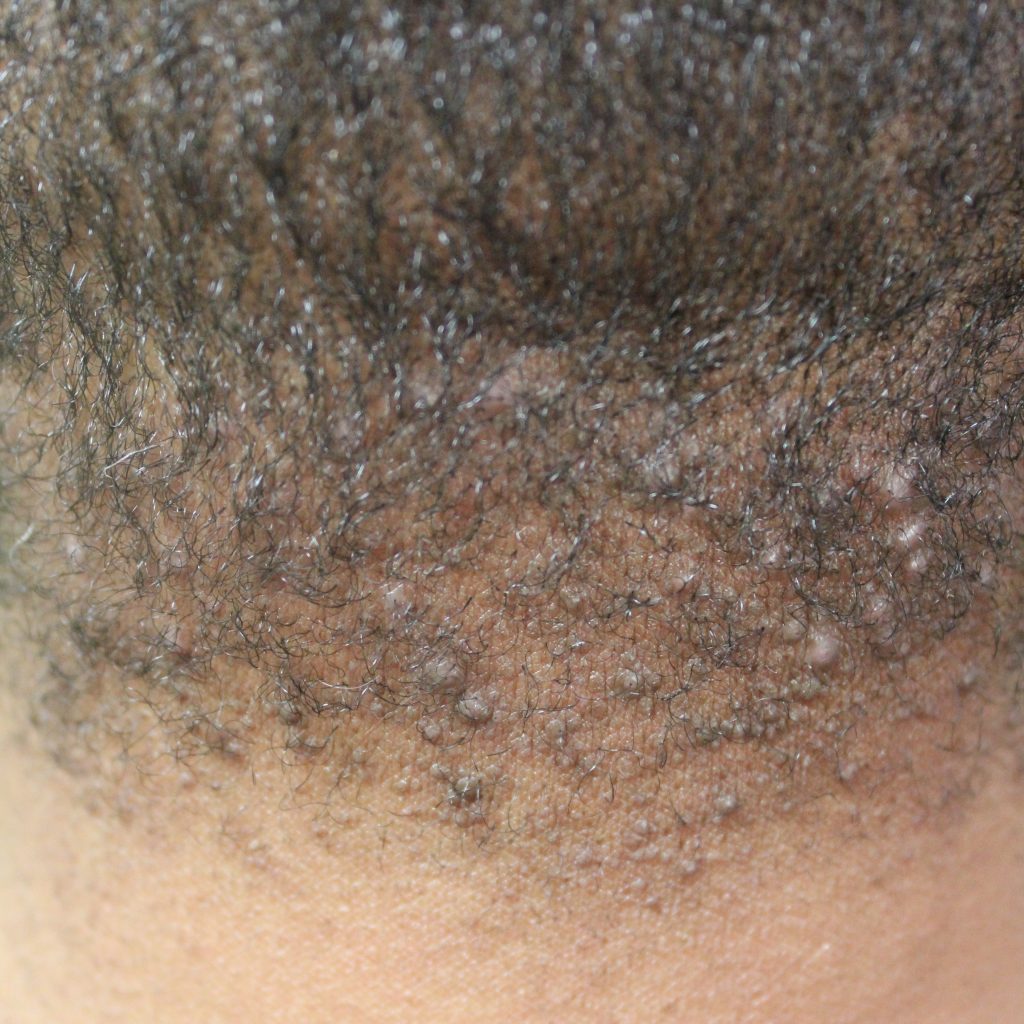
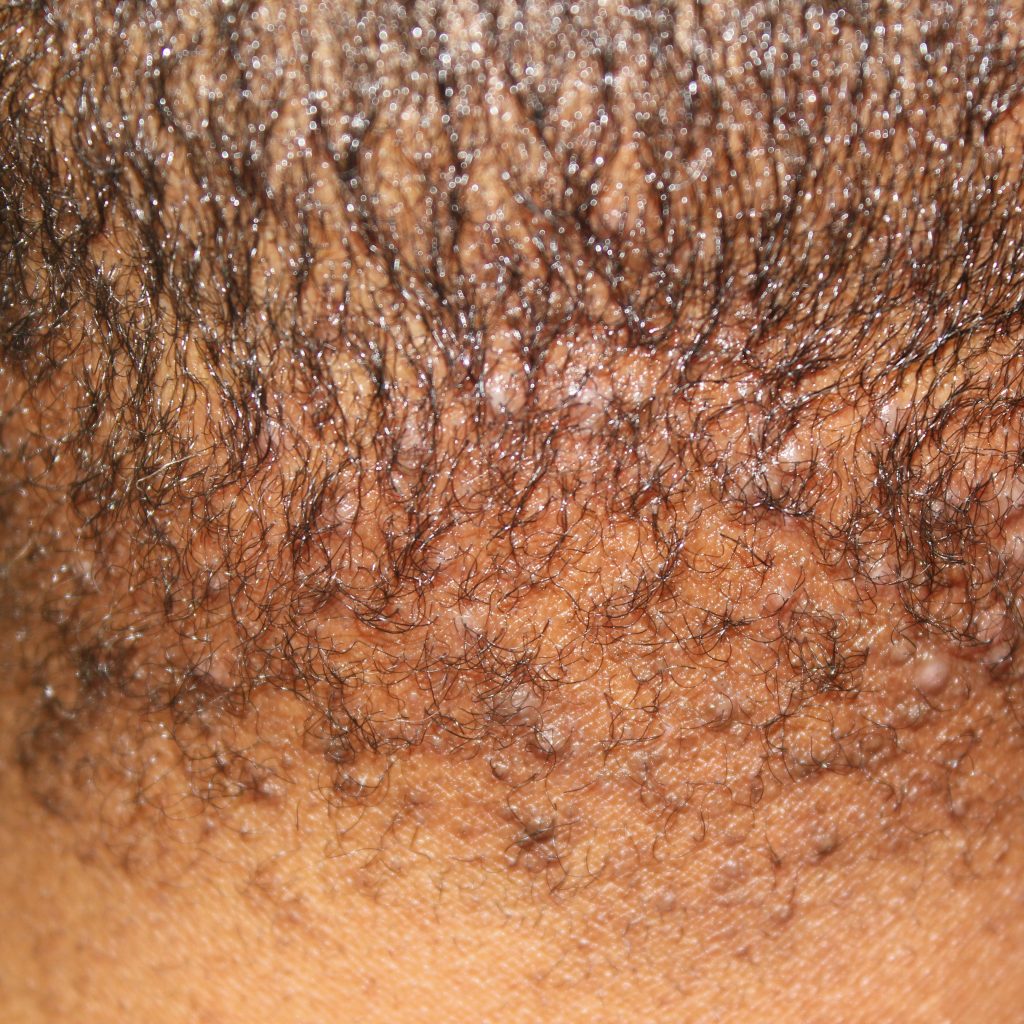
Acne Keloidalis Nuchae (AKN), also known as ‘Acne keloidalis’ or ‘Folliculitis keloidalis,’ is a long standing disease where hair follicles become inflamed and develop bumps and scars on the skin of the back of the head and neck.
A Look At Possible Causes of Acne Keloidalis Nuchae
The exact causes of AKN are not clear. However, the condition has been attributed to a few possible causes.
Autoimmune Issues
Acne Keloidalis Nuchae may be due to the failure of the immune system to distinguish between the individual’s own hair and foreign, invading pathogens. Therefore, the body will start to launch an attack on the hair shaft, in addition to the follicle and sebaceous oil glands. When bacteria propagates, the inflammation becomes more intense as the immune system tries to attack both the microbes as well as the hair shaft.
Although the regrowth of curly hair into the skin is one trigger of the inflammation, the immune system may also react adversely to straight hair. This is evident in patients who suffer from AKN even though they don’t have a curly hair texture.
The inflammation reaction causes the skin to develop bumps. And thick scar tissue then forms as the skin tries to heal itself and repair tears. This is called fibrosis. Collagen producing cells called fibroblasts produce the scar tissue seen in AKN patients. The hair follicle then becomes distorted and occluded (blocked). This is how the hair shaft remains stuck below the skin’s surface, perpetuating an ongoing state of inflammation and scarring.
The immune system continues it’s attempt to attack and destroy healthy tissue by signaling various types of internal defense cells such as neutrophils and lymphocytes. Hypertrophic scar tissue then develops from this, creating large plaques.
Environmental Factors – Do They Cause Acne keloidalis Nuchae
Many sources of information suggest that Acne Keloidalis Nuchae is caused by close shaving, skin friction and irritation from collars and athletic wear. These environmental variables break the hair and encourage the highly curled shafts to grow back into the skin.
According to Hertzberg et al, these external factors are likely to be causes of AKN. This assumption has some degree of support from one study which shows that in 90% of individuals affected, the symptoms started to emerge after using an electric razor to shave the head.
According to Dr U, mechanistic basis for this assumption are indirect and could include:
- Close shaving with a razor would on the account of many patients preceded the emergence of the first lesions
- In most patients the initial lesions; the worst lesons or even the entire lesion is located in skin fold areas of the back of the nape of the head were skin rub s against skin thus after a close shave, the initial stubble that grows out is likely to stab into and irritate the opposing skin fold thus initiating and aggravating the condition. A vicious circle of injury-iriritation-bumps-shave-injury is set and self perpetuated
- Many of the affected patients have co-existing condition of razor bumps in the beard area from shaving closely with razors
- Many of the same treatment approaches for razor bumps in the face such as laser hair removal, skin resurfacing cream such as the retinoids may have some value in very early stages of acne keloidalis nuchae
- The same demographic that is worse affected by razor bumps ( i.e person of African Heritage) are also worse hit by the incidence of acne keloidalis nuchae
However, it should also be noted that other studies were conducted which showed no evidence of ingrown hair as being the cause of Acne Keloidalis Nuchae.
Hormonal Etiology or Cause of Acne Keloidalis Nuchae – AKN
Dr U is of the strong opinion that there is a fundamental hormonal basis for acne keloidalis nuchae rooted in the same hormone implicated in the causation of acne namely DHT. The possible association is based on the following observations;
- Many of these patients have a co-existing conditions known to have a DHT connection, namely: Acne, dissecting cellulitis, follicular occlusion triads etc
- Some of the same treatments that addresses some DHT associated conditions have been useful in some cases of acne keloidalis nuchae
- It is predominantly a disease of males with an overwhelming 20:1 male to female gender distribution
Bacterial Infections and AKN
It is also thought that bacterial infections may damage the hair follicles. According to this hypothesis AKN symptoms result from this, which may explain the formation of pustules as well as the itching and burning which results from this. In Dr U’s opinion there is very little role for bacteria in the etiology of AKN. While secondary infections can occur, it is a rare phenomenon. The pustules in AKN are typically mere end point manifestation of sterile inflammation.
Cylosporine
Although the occurrence of Acne Keloidalis Nuchae in Caucasian individuals is extremely rare, it has been reported to rarely occur in white patients after taking a drug called Cyclosporin.
This prescription is an immunosuppressant which is given to organ transplant recipients. Cyclosporin suppresses the immune system to keep it from harming the new tissue.
Mast Cells
The back of the head where Acne Keloidalis Nuchae tends to develop is an area that has a high concentration of mast cells. These are cells that work as part of the immune system which are intended to attack foreign bodies.
It is possible that sufferers of AKN have a much higher number of mast cells in the occipital region of the head. This may explain why the skin overreacts in response to the individual’s own hair and develops the symptoms that characterize Acne Keloidalis Nuchae.
Who Gets AKN and How Does One Get It?
Acne keloidalis nuchae is a destructive and painful scarring and irritation of the scalp.Researchers show that Acne Keloidalis Nuchae typically affects men, ages 13-25 of African decent because they are more likely to develop tightly curled coarse hair which is kept short. The condition accounts for 0.45% of all instances of dermatosis within this population.
Many experts believe that the regrowth of hair back into the skin causes irritation. This is how follicultis develops, ultimately swelling the follicles then creating lesions and keloid-like scarring.
Cutting the hair short is usually not the issue, but if the hair is short and shaved, this would cause some concern since the tips of the hair have to be close to the skin for it to become ingrown.
On a less frequent basis, AKN may also affect Hispanics and Asians. However, these incidents are comparably minimal compared to males of African descent. Acne Keloidalis Nuchae may also occur in whites. But this is extremely rare. The ratio of men to women with the skin condition has been estimated to be 20:1.
What Happens If I Have Acne Keloidalis Nuchae?
AKN is considered a form of folliculitis, where hair follicles suffer from inflammation. However, there are other more distinctive symptoms which are particular to AKN. This includes:
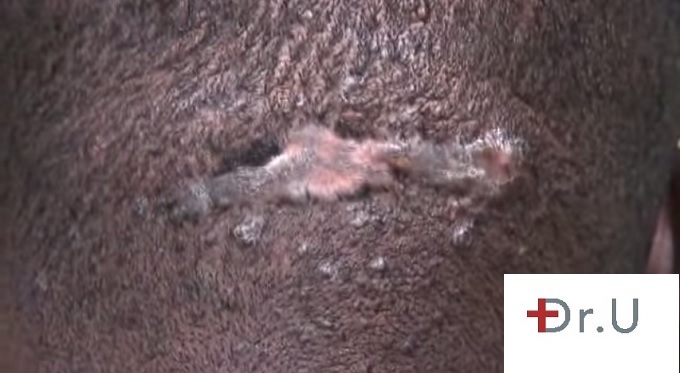
(1) formation of thick scars
(2) development of bumps known as papules and pustules (filled with discharge)
Acne Keloidalis Nuchae starts out as bumps which eventually join together into a single mass of tissue if the condition continues to persist without treatment. The occipital region of the scalp (base of skull) as well as the posterior region of the neck is where AKN tends to manifest. For hair that manages to grow in these areas, they often become ingrown or broken. In more severe cases, the hair can often be permanently lost in areas of widespread inflammation
Besides it’s cosmetic appearance, AKN can feel painful or become itchy (pruritus). And in more severe stages a clear, pus or bloody discharge may start to leak from the affected areas.
Acne Keloidalis Nuchae is both chronic and distressing. The discomfort associated with the development of this condition can interrupt daily life, both emotionally and physically. However, it may be a relief to know that the keloid-like scarring is benign.
Treatment Options for Acne Keloidalis Nuchae also called AKN
Common treatments for Acne Keloidalis Nuchae include the following interventions:
NON SURGICAL Treatment Options for AKN
These are usually good for temporary remissions
- Topical steroids to combat inflammation (e.g. high potency steroids eg clobetasol, temovate etc) Improvements are usually temporary
- Antibiotics such as clindamycin, erythromycin and rifampicin (usually taken for 3 months) which may be helpful in cases where drainage is occurring
- Oral prednisone combined with systemic antibiotics which can be used when drainage or large abscesses are present. Usually, this is taken for a recommended time frame of 4-5 days.
- Oral Isotretinoin has been used when the condition is rapidly progressing
- Triamcinolone acetonide (concentrations of 3-5 mg/mL to 40mg/mL) may be injected into the early stage papules of AKN. Lidocaine-prilocaine may be given 2 hours before the triamcinolone acetonide if pain is a concern. It is often administered through an occlusion made from plastic film.
- Intralesional injections with steroids
- Non ablative laser treatments: These include long pulse ND YAG and Diode lasers. They are useful in early papular stage disease
LONG PULSED ND:YAG LASER TREATMENT OF EARLY ACNE KELOIDALIS NUCHAE
The type of treatment that will be recommended for specific patient presentations will depend on the stage of the condition. Very early forms of the AKN condition may benefit from treatment with Long pulse ND;YAG laser. Studies have shown this the long pulse ND:YAG to be effective in treating papular and even plaque stages of the AKN disease. In a study of 16 patients each treated in 5 sessions at a monthly interval, remission was over 90% in papular AKN after 5 treatments . Flat plaque disease showed 70% improvement with flattening of the plaques.
The theory behind the working of ND YAG long pulsed laser is predicated on the notion that AKN is initiated by an ingrown hair scenarion (as previously discussed). The laser works by removing the offending hair or making it thinner and weaker to the extent that it lacks the ability to cut into the skin to initiate the cycle of hair stab-irritation-tissue fibrous response …
Dr U uses the ND;YAg laser for papular AKN with good results. The following are photos of Dr U’s patient who was treated in this way:
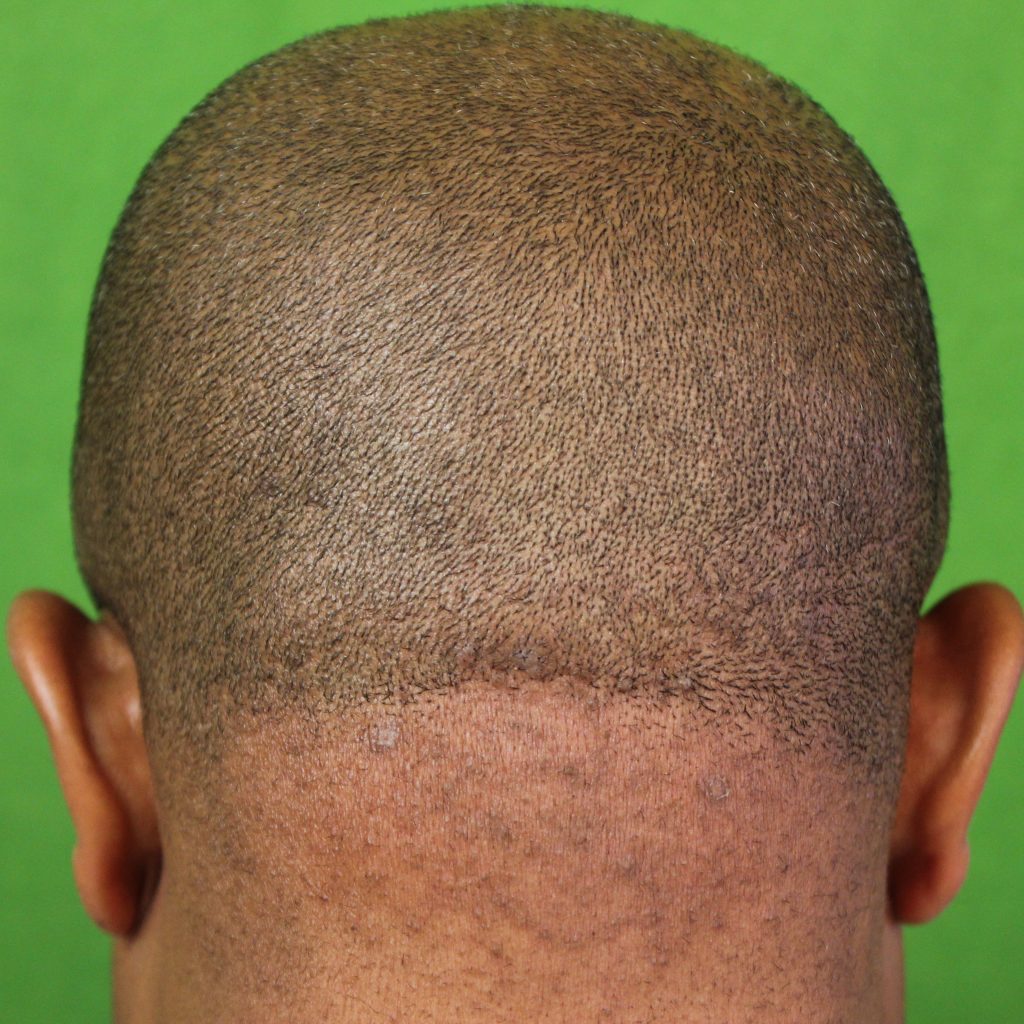
Early stage papular Acne keloidalis nuchae 2 year result after treatment with long pulsed ND YAG Laser by Dr U*
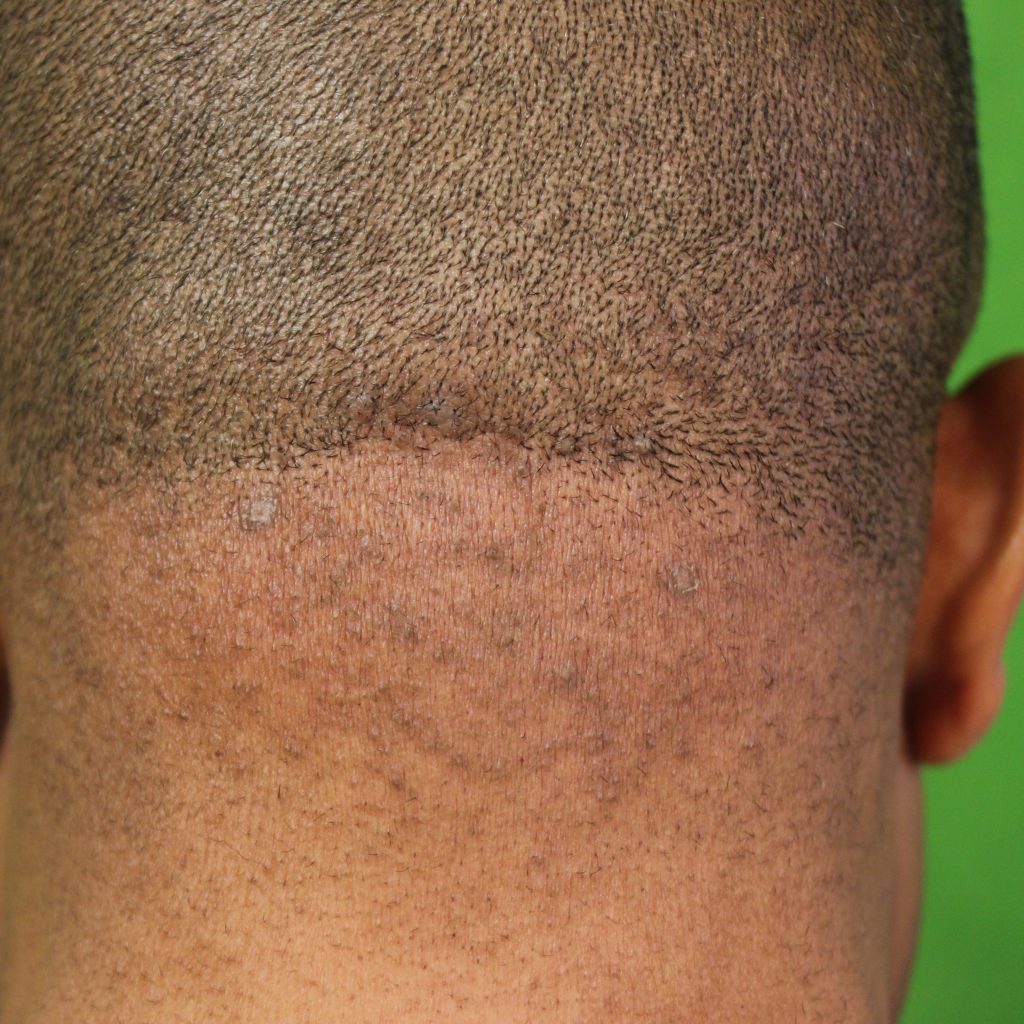
Close up view showing long term remission of papular AKN 2 years after treatment with ND:YAG laser by Dr U*
SURGICAL AND ABLATIVE TREATMENTS
- Radiotherapy can be used to remove the problematic hair which triggers the AKN symptoms as well as arrest growth of scar. The risk of radiation complications makes this treatment option less palatable
- Cryotherapy involves freezing and thawing the AKN tissue in order to remove it. It has been effective for certain types of cases. Even if effective, it would leave behind a large plaque of alopecia (Baldness)
- Vaporisation or laser excision with CO2 laser. Again it is used to ablate or excise the lesion. It would leave a large area of scarred bald area
- Surgical Excision (See below for details)
In most cases, the type of treatment selected is contingent on the stage of the Acne Keloidalis Nuchae symptoms and other factors. For example, laser treatments may be promising for cases where hair is perpetuating the condition. The laser energy works to force the follicle to enter the telogen resting phase and release the hair shaft, a process similar to laser hair removal.
While drugs can help to alleviate uncomfortable symptoms, the most effective way to get rid of the Acne Keloidalis Nuchae bumps or tumor is to surgically remove the unwanted tissue. Dr. U has developed highly specialized surgical techniques to excise AKN lesions, minimize scarring, allow the wound to close over time and even position the horizontal linear scar so that it is aligned very discretely along the posterior hairline. By Using his signature “batman” incision, he creates a hairline that is closer to normal than the typical fish-mouth shaped scars often seen following AKN removal surgeries
To view before and after photos and videos of actual patients, please view our results gallery here.
When the symptoms of AKN start to become evident, it is essential for patients to seek treatment right away to prevent the bumps and scar tissue from becoming larger over time. At later stages, the condition is much harder to reverse.
A Closer Look At The Surgical Removal of Acne Keloidalis Nuchae
Surgery is the most reliable way to actually get rid of tumors and plaques. For this to be successful, the excision needs to be deep enough to reach and remove the affected follicles and the base of the keloidal tissue.
There are several types of surgical and wound healing methods which are commonly used for these types of procedures.
- Excision with primary closure
- A combined approach of excision and grafting
- Staged excision using primary closure
- Electrosurgical excision
- Excision where the wound is closed with a primary closure method
- Excision using secondary intention healing
- Trichophytic closure following excision.
Excision with Primary Closure
With this technique, the affected region is surgically removed as an elliptical shape. The edges are immediately stitched together. This approach will leave a very large and noticeable scar.
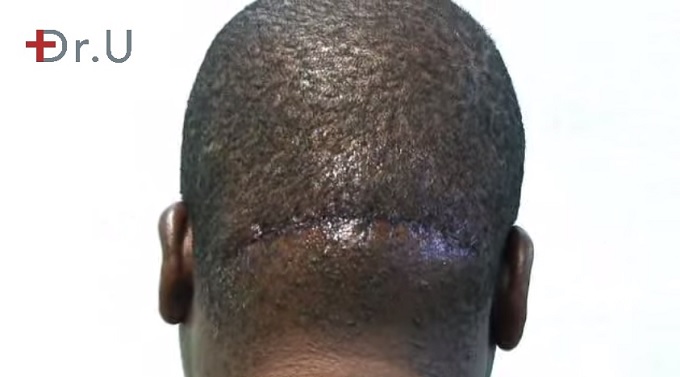
Dr. U successfully removed the Acne Keloidalis Nuchae tumor, leaving a discreet linear scar in its wake.*
Excision with Secondary Healing
Dr U has innovated and pioneered a surgical technique that minimizes scar deformities, hairline deformities and optimal closure using a variation of this approach including new excision strategies including the batman incisions to assist wit the creation of an aesthetically pleasing hairline in the back of the neck upon wound closure. results are evident in the videos shown on this page. Using this strategy, the resulting wound is given about 6-10 weeks to heal following the excision of the unwanted tissue mass. The scar then becomes much smaller and flatter.
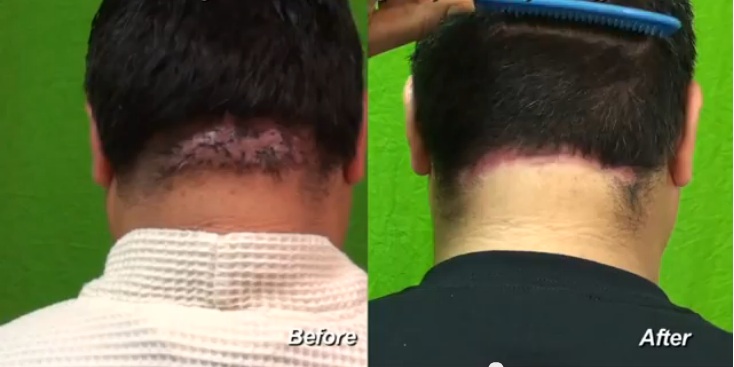
Papular stage Acne Keloidalis Nuchae before and after Dr U Batman Excision with second Intention Closure*
The use of skin grafts to replace the AKN mass of tissue is another possibility. However, this approach is only viable at the theoretical level. In 2011, Beckett, Lawson and Cohen et all noted that this produces poor cosmetic outcomes. What usually happens is that the grafted skin fails to blend in with the surrounding areas.
Acne Keloidalis Nuchae Staged Excision With Primary Closure
With this method, the wound closes in progressive stages. The purpose of this is to enable the patient’s head to move more freely. On the other hand, the range of movement is more restricted when the wound is immediately closed after the excision. Another version of this is excision with trichophytic closure. Using this wound closure approach, the linear scar aligns with the lower hairline at the base of the skull. The line gradually becomes less visible as the hair continues to grow following surgery.
AKN Electrosurgical Excision
With this technique, an electrified wire is used to remove the AKN tumor. The heat causes the blood to solidify through a process referred to as hemostasis. Thus the blood vessels close without a need to tie them off. Therefore, the benefit of using this approach is to reduce bleeding. The wound is given time to heal on its own after gauze and petroleum is applied. Antibiotics are also given to prevent infections.
Patient VIDEO Example of Acne Keloidalis Nuchae Surgery Performed With Trichophytic Closure
Dr. U, who is a board certified dermatologist and a globally renowned hair transplant surgeon combines his skills to deliver the best possible results for AKN patients who choose surgery to get rid of their lesions. The techniques he employs includes:
- serial excisions
- posterior hairline migration
- trichophytic closure
Here is a patient example where the final outcome reflect the use of these different methods. This gentleman suffered from Acne Keloidalis Nuchae for over eight years. He tried steroid injections. But these were not effective. Dr. Umar removed the enlarged tissue mass and strategically positioned the wound so that it would form a linear scar in line with the posterior hairline to make it less noticeable.
Watch this video to learn more about this patient’s story.
In this patient’s example, excision was also followed by a trichophytic closure technique. This individual suffered from Acne Keloidalis Nuchae for six years. He was prescribed oral medication which was quite ineffective although the patient had taken it for six months. Dr. U re-positioned and lowered the posterior hairline so that the linear scar would gradual be covered by hair.
More Videos Depicting Dr Umar’s Successes In Surgically Curing Acne Keloidalis Nuchae – AKN
Here is a second case study of a patient treated with surgical excision second intention healin closure to remove the tumor like mass. This patient had Acne Keloidalis Nuchae for 6 years and was taking prescription oral medication for six months without experiencing any results. Dr. Umar managed to re-position and lower the posterior hair line of this patient so that the scar would eventually be covered by his hair.
Acne Keloidalis Nuchae first emerges as bumps on the back of the head and neck. At the early stages of the condition, patients can still opt for surgery to have pustules and papules removed. Here are two real life examples.
Also if the initial bumps are caused by hair shafts, it is possible to see significant improvement through the application of laser energy.
Surgery remains an option for both early and advanced manifestations of Acne Keloidalis Nuchae. Patients need to discuss their options with a dermatologist who specializes in the condition and weigh the pros and cons carefully.
Other names of Acne Keloidalis Nuchae (AKN):
- AKN
- Acne Keloidalis
- AK
- Dermatitis Papillaris Capillitii
- Folliculitis Keloidalis Nuchae
- Sycosis Nuchae
- Acne Keloid
- Keloidal Folliculitis
- Lichen Keloidalis Nuchae
- Folliculitis Nuchae Scleroticans
- Sycosis Framboesiformis
HISTORY
The first documented case of Acne Keloidalis Nuchae was recording during the 1800s. It underwent several name changes prior to it’s current scientific nomenclature.
1860– sycosis framboesiformis (Hebra)
1869– dermatitis papillaris capillittii (Kaposi)
1872– acne keloidalis (Bazin)
See more results of Acne Keloidalis from Dr U in our youtbe video playlist